Advanced Robotic & Laparoscopic Surgery by Dr. Lovedeep Singh Chauhan
Endometrial cancer, commonly referred to as uterine cancer, is one of the most frequently diagnosed gynecological cancers in women. With increasing awareness, improved diagnostic tools, and advancements in minimally invasive surgical techniques, outcomes have significantly improved—especially when detected early.
Dr. Lovedeep Singh Chauhan, Consultant Surgical Oncologist at Max Super Speciality Hospital, Mohali, provides comprehensive, evidence-based treatment for endometrial cancer using advanced robotic and laparoscopic techniques. The goal is not only complete cancer removal but also faster recovery, minimal complications, and long-term quality of life.
Understanding Endometrial (Uterine) Cancer
The uterus is a hollow, muscular organ located in the pelvis. Its inner lining, called the endometrium, thickens and sheds during the menstrual cycle. Endometrial cancer begins when abnormal cells in this lining grow uncontrollably.
It is important to understand that “uterine cancer” is often used interchangeably with “endometrial cancer,” although technically, uterine cancer can include rare tumors of the uterine muscle (sarcomas). However, the vast majority of uterine cancers arise from the endometrium.
One of the most reassuring aspects of endometrial cancer is that it frequently presents early, often through abnormal vaginal bleeding. This early warning sign allows timely diagnosis and treatment, leading to excellent survival rates in early-stage disease.
Types of Endometrial Cancer
Endometrial cancer is broadly classified into two major categories based on pathology and behavior.
Type I – Endometrioid Adenocarcinoma
This is the most common type. It is often associated with prolonged exposure to estrogen without progesterone balance. It tends to grow slowly and is usually diagnosed at an early stage. The prognosis is generally favorable.
Type II – Non-Endometrioid Cancers
These include serous carcinoma, clear cell carcinoma, and carcinosarcoma. These tumors are biologically more aggressive and may spread earlier. They require more intensive treatment planning and closer follow-up.
Accurate histopathological classification plays a critical role in deciding the extent of surgery and the need for additional therapy such as chemotherapy or radiation.
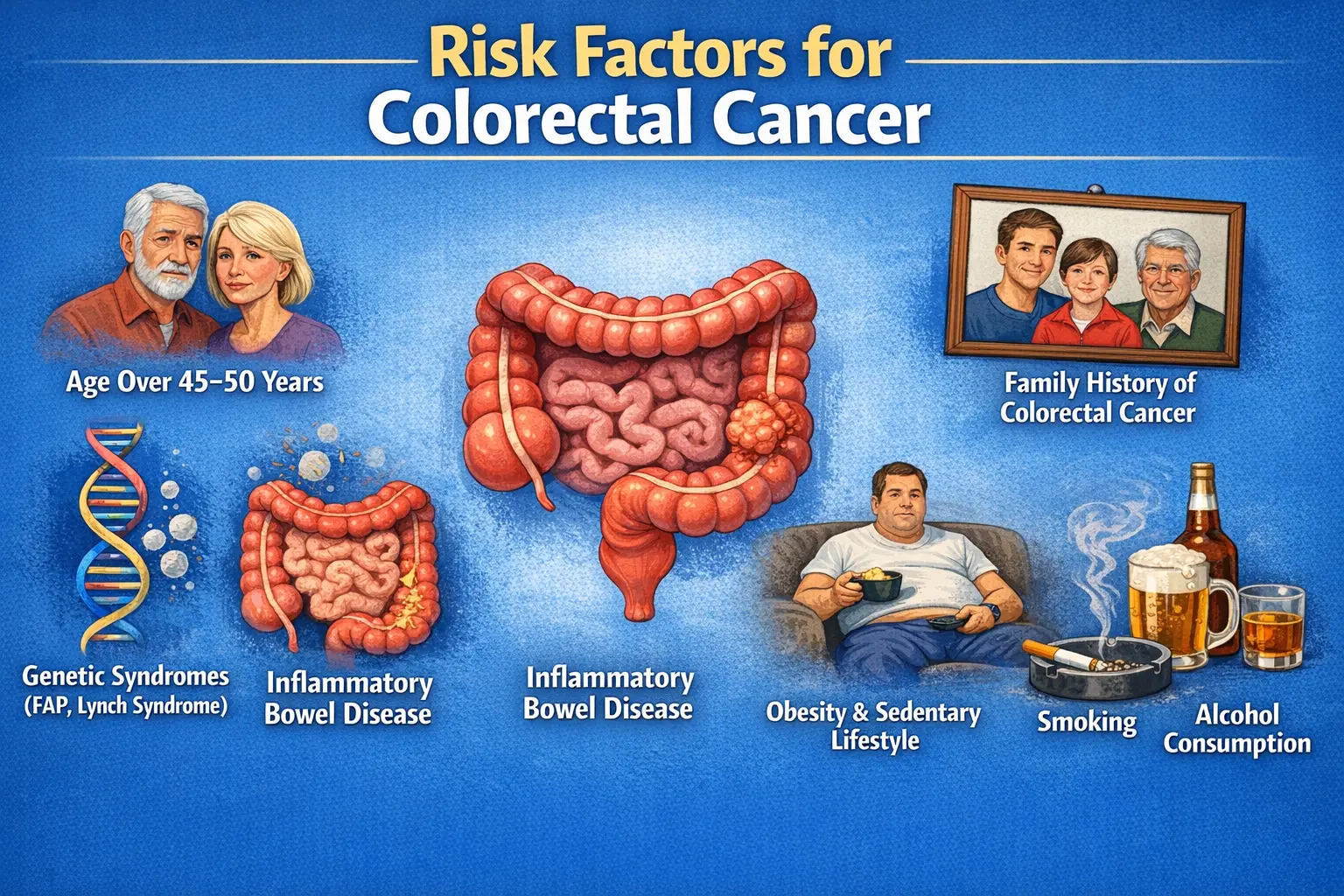
Risk Factors and Causes
Endometrial cancer develops due to a combination of hormonal, metabolic, genetic, and lifestyle factors.
Women with obesity have a significantly increased risk because excess body fat converts androgens into estrogen, leading to prolonged endometrial stimulation. Diabetes and hypertension are also frequently associated.
- Early onset of menstruation or late menopause
- Nulliparity (never having given birth)
- Polycystic ovarian syndrome (PCOS)
- Use of estrogen-only hormone replacement therapy
- Family history of hereditary cancer syndromes such as Lynch syndrome
While these factors increase risk, many women diagnosed with endometrial cancer may not have identifiable risk factors. Regular gynecological evaluation and prompt attention to abnormal bleeding remain crucial.
Symptoms of Endometrial Cancer
Abnormal vaginal bleeding is the hallmark symptom. In postmenopausal women, even a single episode of bleeding warrants immediate medical evaluation.
- Heavy or irregular menstrual bleeding in premenopausal women
- Pelvic pain or pressure
- Unusual vaginal discharge
- Pain during intercourse
Because symptoms often appear early, many patients are diagnosed before the cancer spreads beyond the uterus.
Diagnostic Evaluation and Staging
Accurate diagnosis and staging form the foundation of effective treatment planning for endometrial cancer.
Diagnostic Evaluation
The diagnostic process usually begins with a transvaginal ultrasound to measure endometrial thickness. If suspicious findings are present, an endometrial biopsy is performed for histopathological examination.
- MRI of the pelvis to assess depth of myometrial invasion
- CT scan of the abdomen and chest to detect spread
- PET-CT in selected high-risk cases
- Molecular testing for high-risk or recurrent disease
Staging (FIGO System)
Staging is primarily surgical and evaluates tumor spread to guide adjuvant therapy decisions.
- Tumor confined to the uterus
- Depth of invasion into the muscle layer
- Involvement of cervix
- Lymph node spread
- Distant metastasis
Comprehensive surgical staging ensures accurate risk assessment and optimal treatment planning.
Treatment of Endometrial Cancer
Treatment depends on stage, tumor grade, histological subtype, and overall patient health. Management is individualized after multidisciplinary discussion.
Surgery – The Cornerstone of Treatment
Surgery remains the primary and most important treatment for endometrial cancer. Standard procedures include:
- Total hysterectomy (removal of uterus)
- Bilateral salpingo-oophorectomy (removal of ovaries and fallopian tubes)
- Pelvic and para-aortic lymph node assessment
- Omentectomy in selected high-risk cases
Minimally Invasive & Robotic Surgery
Dr. Lovedeep Singh Chauhan specializes in laparoscopic and robotic techniques, offering benefits such as:
- Smaller incisions
- Less postoperative pain
- Reduced blood loss
- Lower infection risk
- Faster recovery
- Shorter hospital stay
Robotic-assisted surgery allows enhanced precision, better visualization, and improved lymph node dissection accuracy, particularly in obese or high-risk patients.
Adjuvant Therapy
Depending on surgical findings and risk stratification, additional treatment may be recommended:
Radiation therapy to reduce local recurrence
Chemotherapy for high-grade or advanced-stage tumors
Hormonal therapy in selected early-stage, low-grade cases
Targeted therapy or immunotherapy in recurrent or metastatic disease
Treatment decisions are individualized and discussed thoroughly with the patient and family.
Fertility Preservation in Selected Patients
In young women with early-stage, low-grade tumors confined to the endometrium, fertility-sparing management using hormonal therapy may be considered under strict surveillance.
Such decisions require careful evaluation, counseling, and regular endometrial assessment to ensure safety.
Recovery After Surgery
Recovery after minimally invasive surgery is generally smooth. Most patients are mobilized within 24 hours and discharged within a few days.
Postoperative care focuses on:
- Early ambulation
- Pain management
- Prevention of blood clots
- Gradual return to normal activities
Full recovery usually occurs within 2–4 weeks for minimally invasive surgery, compared to longer recovery after open surgery.
Recovery After Surgery
Recovery after minimally invasive surgery is generally smooth. Most patients are mobilized within 24 hours and discharged within a few days.
Postoperative care focuses on:
- Early ambulation
- Pain management
- Prevention of blood clots
- Gradual return to normal activities
Full recovery usually occurs within 2–4 weeks for minimally invasive surgery, compared to longer recovery after open surgery.
Long-Term Follow-Up and Survivorship
Follow-up care is essential, especially during the first three years when recurrence risk is highest. Regular visits include:
- Clinical examination
- Imaging when indicated
- Monitoring of symptoms
- Counseling regarding lifestyle and weight management
Survivorship care also addresses emotional well-being, menopausal symptoms, bone health, and overall quality of life.
Why Choose Dr. Lovedeep Singh Chauhan for Endometrial Cancer Treatment?
Choosing the right surgical oncologist significantly influences outcomes in gynecological cancers.
Dr. Lovedeep Singh Chauhan is a highly trained Surgical Oncologist with specialized expertise in minimally invasive and robotic cancer surgery. His approach combines oncological safety with organ preservation whenever appropriate.
At Max Super Speciality Hospital, Mohali, patients benefit from:
- Advanced robotic surgical platform
- Dedicated oncology operation theatres
- Multidisciplinary tumor board discussions
- Evidence-based treatment protocols
- Comprehensive ICU and postoperative support
Each treatment plan is personalized, ensuring that patients receive optimal therapy tailored to tumor biology and overall health status.
When Should You Consult a Surgical Oncologist?
You should seek expert evaluation if you experience:
Postmenopausal bleeding
Persistent abnormal menstrual bleeding
Suspicious findings on ultrasound
Newly diagnosed endometrial cancer
Need for a second opinion
Early consultation allows accurate staging and timely initiation of treatment, improving survival and quality of life.